Orthopaedic Expert Care You Can Trust

Prior to starting the procedure, the patient is placed on a traction table. There is a well-padded post in between the legs and the legs are in a ski boot type device, which allows us to pull on the leg whilst maintaining your body in the same position (traction). This creates room to place the camera through an incision into the hip joint. Through the second incision the instruments are placed, sometimes a third incision is needed. And x-ray machine is used throughout the procedure to confirm correct placement of instruments and adequate excision/trimming of bone.
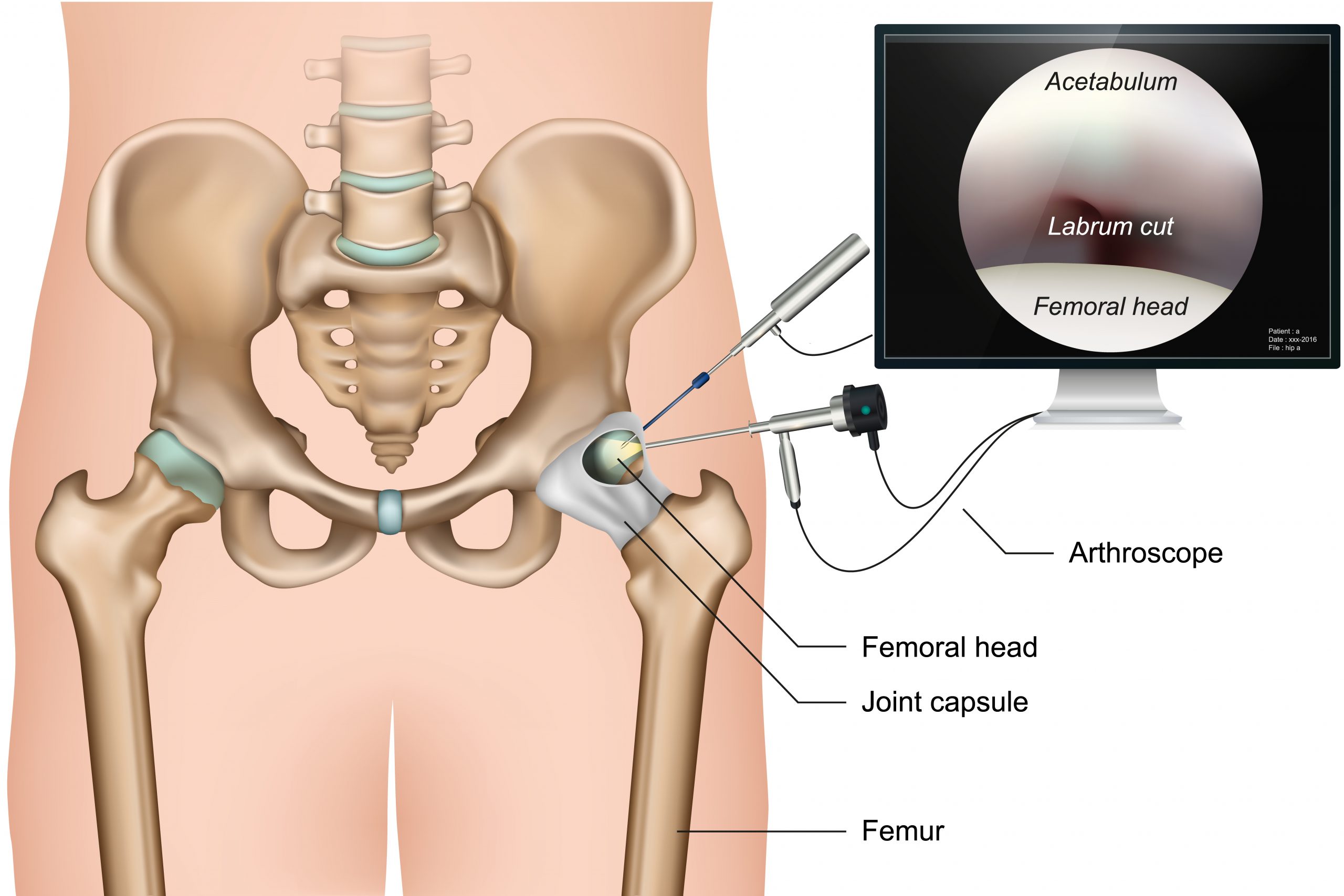
ACTUAL VIDEO OF THE EXCESS BONE BEING TRIMMED
The operation can take anything from 1.5 to 3 hours and depends on how much work needs to be done in the hip joint. The surgical scars are small, however there may be considerable swelling after the procedure as a lot of fluid is run through the hip joint and some of this can be absorbed in the skin and muscle. Rest assured, over the course of the next two weeks this all subsides.
Hospital stay
I usually perform the hip arthroscopy as a day procedure. This means that the surgery occurs in the morning and patients go home later on that afternoon or evening. Occasionally patients may need to stay in overnight if pain control is an issue. Most patients walk with the aid of crutches but I allow them to put all their weight on the leg. Very rarely do I need to restrict the amount of weight placed through the leg. Most patients use one or two crutches for a week or two. The minimum period I advise my patients to be off work is two weeks. Depending on how you commute to work this may increase to 6 weeks.
Rehabilitation
The key to success following surgery is rehabilitation. Frequently, I ask my patients to see a good physiotherapist with a “pre-habilitation” program. This is to condition the muscles so that they are at their optimum prior to surgery. Following surgery, rehabilitation protocols are essential. My patients do pendulum exercises on the same day of surgery. If possible, the use of a static bike from the next day is very useful to prevent stiffness and maintain range of motion. Supervised physiotherapy is then undertaken and the rehabilitation is a commitment. After the intial phase of stretching and strengthening, patients progress to stamina and sports specific rehab. We can discuss this in detail if we decide this is the correct operation for you. It can take 4-6 months to fully recover from this procedure.
Why do we perform hip arthroscopy?
There are three main reasons why I perform hip arthroscopy.
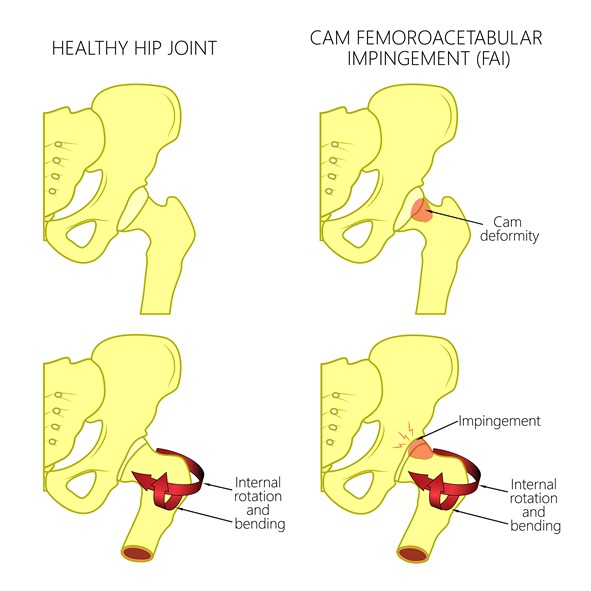
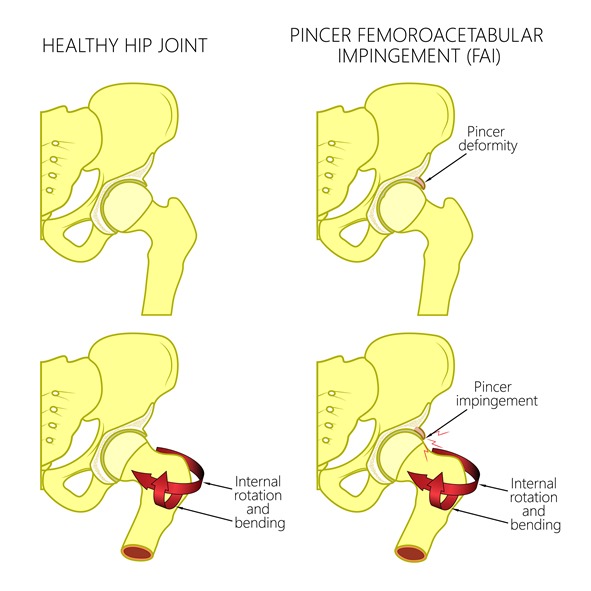
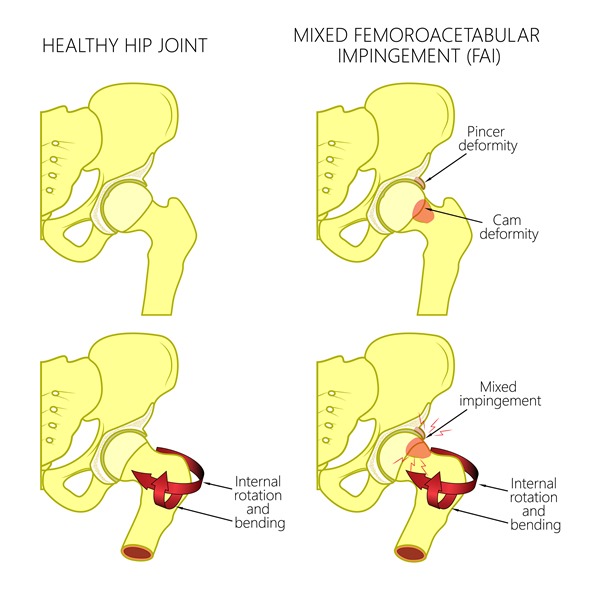
Femoroacetabular impingement (FAI) (or Hip Impingement)
There are two main types of hip impingement. In cam hip impingement there is excess bone around the ball of your femur. In pincer hip impingement the socket is overgrown and covers more of the ball. In mixed impingement, both abnormalities exist. In all forms of impingement, patients complain of groin pain when they flex their hips (bring their knee towards the chest). During arthroscopy the excess bone can be shaved thereby allowing smoother movement. I typically perform a dynamic test for residual impingement to ensure I have taken away adequate bone.
Labral tear
The rim of your hip socket is lined with a fibrous cartilage called the labrum. This cartilage is different to the cartilage lining the ball and socket of the hip joint. The labrum serves to keep the fluid inside the hip joint and forms a suction seal. For further information please read my article on ‘your hips don’t lie’.
The labrum can be torn for a variety of reasons. The most common reason is hip impingement. Patients are also prone to labral tears if they have dysplasia of the hip where the socket is not fully developed and doesn’t cover all of the femoral head or ball. The labrum can also be torn in sporting injuries. During hip arthroscopy, I always aim to preserve the labrum and repair if possible. The results have been shown to be better with a repair than the more commonly performed debridement.
Click here to learn more about labral tears
Articular cartilage damage
The cartilage lining the ball and socket of your hip joint is truly a unique structure that nature has provided us with. It’s facilitates smooth movement of the joint that is fiction free. This cartilage can be torn as a result of hip impingement or simply just trauma from activities that involve running or jumping or pivoting. A number of techniques can be used to address this during hip arthroscopy.
Complications and surgical risks
All surgery carries risks, which can be generalised or specific to the surgery. General complications include things related to the general anaesthesia, for example, inability to pass urine , blood clots in the legs or lungs, and infection can occur with any surgical procedure, but is extremely low following hip arthroscopy.
Specific risks to hip arthroscopy include
- nerve damage, causing numbness on the side of your thigh
- traction injury, causing numbness and bruising in the groin and a foot
- very rarely, damage to the sciatic nerve leading to foot drop
- rarely, the labrum repair fails to heal or gets retorn again
- Sometimes, fibrous bands or adhesions can form in the joint leading to stiffness
We can discuss all of these during our consultation and there will be plenty of time to discuss everything in more detail.
Why choose Mr. Jaiswal?
Not only have I completed a fellowship in a high volume hip arthroscopy centre, but also, I have been a consultant in a highly specialised Young Adult Hip Unit. During this time, I was selected by the British Hip Society to undertake the prestigious Travelling Fellowship in Vail, Colorado (USA) to learn from one of the best hip arthroscopists in the world (Marc Philippon). Thus, you should be reassured, that I have learnt and practice on a regular basis advanced hip arthroscopy techniques to achieve the best possible outcomes for my patients. Currently, I am in the process of setting up a Young Adult Hip Unit at The Royal Free London NHS Trust.
Frequently asked questions
How long does hip arthroscopy take?
The surgery usually takes about an hour and a half to perform. If there is more extensive work required it can take up to 2 1/2 hours. I ensure that the labrum is very stable after I have repaired it and the duration of surgery is longer, if more stitches are required to stabilise it.
How long do I need to stay in hospital?
I usually perform the procedure as a day case. The operation usually occurs in the morning and patients go home the afternoon or evening. Occasionally and especially if patients live far away they may stay overnight. Patients get seen by the physiotherapist in the morning of surgery and before discharge.
What problems are issues can I expect after the surgery
There will be considerable swelling around the hip. The swelling should subside over the next 2 to 3 weeks. There may also be some bruising and certainly you will experience some discomfort. There may be some numbness around the groin thigh or foot area and the ankle may be sore. There may be some leakage from the wounds and if this persists for more than 2 to 3 days then you should contact my practice.
You will require two crutches and usually patients have them for a week and then one crutch for the second week. Depending on how I have repaired the labrum, your hip movements may be restricted to 90°. You’ll be encouraged to use a static bike from day one to get the hip moving and prevent stiffness. Pendulum exercises should be performed from the evening of the surgery and the physiotherapist will show you what to do and how to do it.
Can I shower with my dressings on?
You will be discharged with waterproof dressings and therefore you will be allowed to shower. We will give you spare dressings in case the ones that were put on after surgery come off.
Can I shower with my dressings on?
You will be discharged with waterproof dressings and therefore you will be allowed to shower. We will give you spare dressings in case the ones that were put on after surgery come off.
When can I drive after surgery?
I usually allow patients to drive after two weeks and when the wounds have healed. You will need to make an assessment of how comfortable you feel in the car. The key factor is the ability to perform an emergency stop and this will need to be tested before going on the road.
When will I need a follow-up appointment?
The stitches will need to come out at two weeks and this is usually done at your general practice by a nurse. I usually like to see my patients six weeks after the operation but this can be changed to a time which is more convenient for you.
When can I travel after surgery?
You can travel when you feel comfortable. For long-distance travel, I advise patients to wait at least six weeks and if possible 12 weeks. This lowers the risk of getting blood clots.